Doctors Can't Recognize Measles Anymore
A hospital's failure to isolate measles patients exposes a generation of doctors unprepared for preventable diseases as vaccination rates decline nationwide.
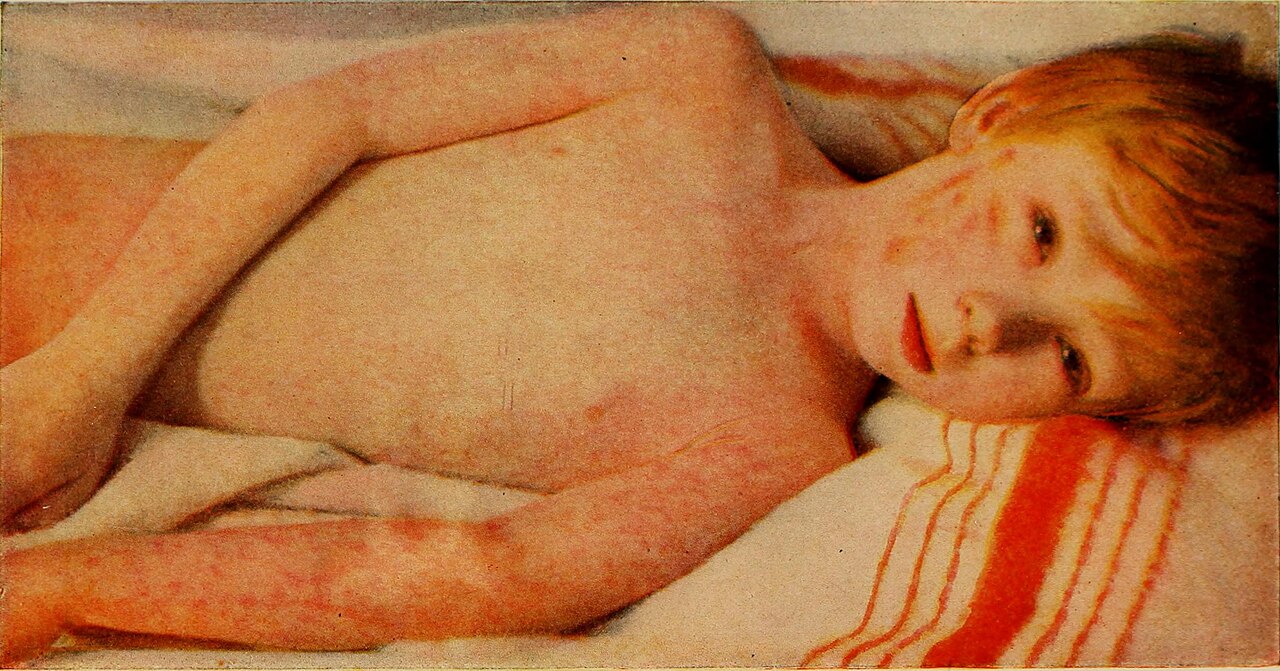
Two hours. That's how long Mission Hospital in Asheville let two measles-infected children sit in an open ER waiting room — unisolated, contagious, and unrecognized — while 26 others breathed the same air before proper isolation occurred.
The Jan. 4 incident earned Mission Hospital "Immediate Jeopardy" status from federal regulators. But this Asheville failure represents something larger than one hospital's oversight. It reveals a generational collapse in American medicine's defenses against preventable diseases that once remained under control.
The Centers for Disease Control and Prevention confirmed 1,575 measles cases nationwide this year, the highest count in a generation. Ninety-two percent of those cases are in unvaccinated individuals or those with unknown vaccination status. Seventy-four percent involve children and young adults up to 19 years old.
"There's a word, 'morbilliform' — it means measles-like, and there are lots of viruses that can cause a rash that looks like a measles rash in children," said Dr. Theresa Flynn, president of the North Carolina Pediatric Society. "In 30 years in health care, I've never seen a measles case."
Dr. Andy Lubell, chief medical officer at True North Pediatrics in Pennsylvania, echoed that assessment. "The generation of physicians who are currently, for the most part, treating patients haven't actually seen what a measles case looks like other than from a textbook or a video," Lubell said.
The clinical ignorance corresponds with an erosion of national guidance. Pediatricians on the front lines report receiving no proactive support from federal health agencies during the outbreak.
"We certainly do not feel the support or guidance from the CDC right now," said Dr. Brigette Fogleman, a pediatrician at Asheville Children's Medical Center. Andrew Nixon, a CDC spokesperson, said state and local health departments "have the lead in investigating measles cases and outbreaks" while the CDC provides support "as requested."
Measles virus can remain airborne for up to two hours after an infected person leaves a room, making the Asheville hospital's two-hour isolation delay potentially catastrophic for exposure. The virus now circulates among healthier, unvaccinated youth who often recover without hospitalization but spread it further.
The national outbreak isn't isolated to North Carolina. Spartanburg County, South Carolina, was the center of an outbreak with 94 percent of the state's 997 cases as of March 27. Only 10 states plus Washington, D.C., maintain the 95 percent MMR vaccination coverage needed for herd immunity. Idaho's vaccination rate stands at 78.5 percent.
Kindergarten MMR coverage dropped from 95.2 percent in 2019-2020 to 92.5 percent in 2024-2025, according to CDC data.
At Mission Hospital, 7-year-old twin brothers arrived at 2 a.m. on Jan. 4 with measles symptoms. Staff moved them from an open waiting room to a 12-patient care area with only plastic partitions. Proper isolation didn't occur until 4:20 a.m., more than two hours after their arrival.
Fogleman recounted a recent conversation that illustrates the public perception problem. "One parent recently told a nurse, 'It's only measles. It doesn't kill anybody,'" she said. "That's not true, her team must explain."
The hospitalization rate tells another story. Five percent of 2026 measles cases required hospital care, down from 11 percent in 2025. Experts say this reflects the virus spreading through healthier populations, not improved outcomes.
The CDC recorded 74 hospitalizations this year. Three measles deaths occurred in 2025 — two children in Texas and one adult in New Mexico.
Dr. Patsy Stinchfield, former president of the National Foundation for Infectious Diseases, delivered a blunt assessment of federal response. "When you are at the highest level of measles cases in 30 years, we should be seeing lots more from our federal government," Stinchfield said. "And I think it's harming kids and causing an inordinate amount of work and expense that really doesn't belong in health care right now."
Scott Thorpe, executive director of the Southern Alliance for Public Health Leadership, warned that Spartanburg's outbreak represents a national pattern. "Spartanburg is not an outlier," Thorpe said. "Just across the border in western North Carolina, there are lots of counties with lower vaccination rates. And we've already started to see some cases there."
Mission Hospital staff received training on measles recognition — the "three C's" of cough, coryza, and conjunctivitis — seven months before the January incident. Yet when symptomatic twins arrived, no one recognized the threat.
The hospital's enhanced correction plan won acceptance from the Centers for Medicare and Medicaid Services on Feb. 2. But the damage extended beyond those 26 exposed individuals.
Buncombe County reported seven measles cases by mid-February, though health officials haven't confirmed how many link to the Mission Hospital exposure.
Michael Osterholm, director of the Center for Infectious Disease Research and Policy at the University of Minnesota, offered a sobering forecast. "There are a lot more South Carolinas waiting to happen," Osterholm said.
As measles cases continue climbing, American hospitals face a dual challenge: treating a disease most clinicians have never encountered while operating within a public health system that redirected resources toward ideological initiatives and pandemic theater. The children in Mission Hospital's waiting room became collateral damage in that larger institutional failure.